Coming In January: Obamacare Rate Shock, Part Two
by Charles Ornstein,ProPublica.
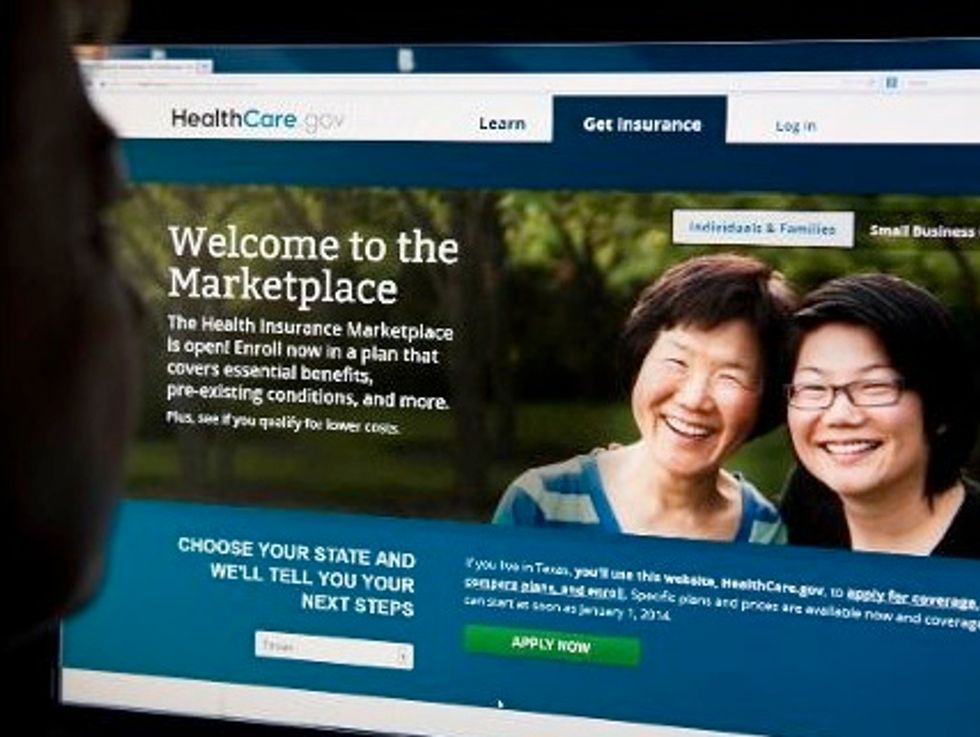
Media reports about the Affordable Care Act have been dominated by two themes lately: The ongoing glitches with Healthcare.gov and the “rate shock” that some consumers now face after insurance companies canceled their policies.
But come January, a second rate shock may hit and could produce more bad news for Obamacare.
That’s when millions of Americans who select health insurance plans on the new marketplaces may realize that their new insurance plans don’t pay the bills right away. They come with high deductibles and co-pays.
In recent weeks, many people have focused on the monthly cost of buying a health insurance plan in the insurance marketplace. What I’m talking about is different: The out-of-pocket costs they may face when they go to use that new policy.
The president has promised to deliver affordable care to all Americans who want it. But the notion of what’s affordable may well be in the eye of the beholder.
Many low-income people who haven’t had insurance before will qualify for subsidies to lower their monthly insurance premiums and reduce their out-of-pocket costs. And some with current policies will find that their new ones are indeed more affordable.
But many won’t. Those on both the left and the right side of the political spectrum — and in between — acknowledge this may surprise consumers.
“So many people may feel they have a grip on their premium costs and think they have reasonable coverage only to encounter unpleasant surprises in the form of deductibles, co-payments, and co-insurance amounts,” health care consultant Kip Piper told me in an email.
Consider a family of four making $59,000 a year. They will have to pay $400 a month toward their insurance premium, after receiving a subsidy, said industry consultant Robert Laszewski.
“But then, they will get a plan with a $2,000 deductible and hefty co-pays,” he wrote in an email. “The Democrats who say everything is going to be OK really need to go on one of the open exchanges and take a hard look at what consumers will see.”
It goes without saying that the Affordable Care Act reshapes the insurance landscape. It prohibits insurers from discriminating against those with pre-existing conditions and requires insurers to spend a minimum amount on health costs vs. marketing and profit.
Beyond that, the act provides subsidies to working-class consumers. Earlier this month, the New York Times boasted that up to 7 million people could qualify for “free” policies under the law. That’s going to cost about $1 trillion over the next decade.
Let’s take a brief, wonky diversion into some technical details (I promise it will be brief).
There are four types of plans being offered on the exchanges: bronze, silver, gold and platinum. As you move up the medal ladder, the premiums generally increase, as do the benefits.
Separately, there are two different kinds of financial assistance provided to people, depending on their income level.
—Those with incomes below 400 percent of the federal poverty rate ($45,960 for one person, $94,200 for a family of four) qualify for tax credits that lower the cost of monthly premiums.
—In addition, those with incomes below 250 percent of poverty ($28,725 for an individual, $58,875 for a family of four) qualify for help with their deductibles and co-pays.
You’ll hear the phrase “actuarial value” used a lot to describe the value of different plans. Essentially this means that a plan is structured to cover a certain percentage (say 60 percent or 70 percent) of the benefits provided to the population it is designed to serve.
OK, wonky diversion over.
A spokesperson for the Centers for Medicare and Medicaid Services, which oversees the marketplaces, said that when consumers apply for coverage, they will receive an eligibility determination detailing whether they qualify for tax credits and a cost-sharing reduction, as well as next steps to take.
But the new coverage won’t be a panacea, experts say. The problems with the Healthcare.gov website, which handles enrollment for 36 states, has made communicating details of the new policies challenging.
“The website difficulties have meant that in much of the country people have yet to really see what the cost-sharing will look like in these plans, and they may be surprised for find out that the deductibles and co-pays in bronze and silver plans are higher than what one would find in typical employer-provided health benefits,” Larry Levitt, senior vice president of the Kaiser Family Foundation, said in an email.
“I think it remains to be seen whether people see these plans as offering them good protection against catastrophic health expenses — which they do — or are disappointed that they won’t generally provide much coverage for occasional visits to the doctor or prescriptions,” Levitt added.
Chris Jacobs, a senior policy analyst at the conservative Heritage Foundation, brings up another point. The sequester law, which calls for spending cuts in the federal budget, requires reductions to the cost-sharing program. But the Obama administration has not said how it will carry those out — whether it will cut the cost-sharing subsidies or make insurers absorb the cuts.
“Someone (either carriers, consumers, or both) isn’t being told by this administration that they’re going to have to pay more — billions of dollars more,” Jacobs wrote to me. “And just as millions of people didn’t like discovering in recent weeks that the ‘like your plan’ promise was hollow, they won’t like learning about other hidden costs not being disclosed either.”
Jacobs has written more about the issue, as has Kaiser.
Ken Wood, a senior advisor to Covered California, the state’s exchange, said that officials tried to structure their plans so they don’t rely on deductibles as much as co-pays. They offer lower co-pays for trips to primary-care physician visits than to specialists and lower co-pays for visits to urgent-care clinics than to emergency rooms.
“Even with high deductibles, consumers stop paying retail for health care since they get the advantage of the health insurer’s negotiated rates, and no plan has a higher out-of-pocket maximum than $6,350 (per person),” he said. “That is a lot of money, but it probably will not drive people into bankruptcy. ”
Has your insurance been canceled? Have you tried signing up for coverage through the new exchanges? Help us cover the Affordable Care Act by sharing your insurance story.
AFP Photo/Karen Bleier


