By Seema Yasmin, The Dallas Morning News
GALVESTON, Texas — In a laboratory on Galveston Island, Tom Geisbert is working overtime.
The pressure is on as the biggest Ebola epidemic in history creeps across West Africa, jumping over borders and permeating cells. The virus has killed more than 1,350 people.
For Geisbert, three decades of scientific grunt work — hours of pipetting and disinfecting and note-taking and grant-writing — are thrust into the limelight. The public demands a cure.
But Ebola treatments poised for human tests have been stuck in limbo for nearly a decade. Now demand for those treatments is high, but the market is small. Before this outbreak, Ebola had killed fewer than 1,600 people since its discovery in 1976.
Any viable options for a cure will pass through Geisbert’s office in Galveston National Laboratory, a square, beige building that sits on the University of Texas Medical Branch campus on the eastern end of Galveston Island.
Here, scientists aren’t the only critical resources. Monkeys are, too, as evidenced by crates of yellow perforated balls in one of the building’s hallways. The balls are stuffed with food and used to entertain the animals as they work for their treats.
Six years ago, Geisbert, 52, a professor of microbiology and immunology, infected monkeys with Ebola and then gave them a vaccine he had developed. The monkeys survived. Two other treatments developed at the Galveston National Laboratory show similar promise.
But so far, none of Geisbert’s inventions have been tested in humans. The scientist is growing frustrated.
___
Looking through a powerful microscope, we meet Ebola. Magnified 60,000 times, the virus appears like a short piece of spaghetti. A stringy, thin tail hangs from an ampersand-shaped coil. Speckling its surface are thousands of three-pronged forks. The forks attach to a human cell, fusing virus to human until they are one.
___
It can cost half a billion dollars to take a vaccine from lab to clinic. Oftentimes, what works in the lab stays in the lab.
The World Health Organization requires an opened vial of vaccine to remain stable and usable for six hours. Many vaccines have stumbled at that step. Others, made in small batches in the lab, cannot be manufactured in large amounts, because of cost and technical challenges.
Besides vaccines, there are two other potential options for treating Ebola.
One interferes with the virus’s genes and stops it from making more copies of itself. The other uses antibodies, molecules that float in the blood and latch onto the virus, tagging it as a dangerous intruder.
An experimental antibody treatment was given to Kent Brantly, a Texas doctor, and Nancy Writebol, an American missionary, both of whom became infected with Ebola in Liberia. Scientists at Galveston National Laboratory collaborated with the small company that made the treatment.
“People worry that Ebola is now in America,” says Jim LeDuc, the lab’s director, referring Brantly and Writebol, who were airlifted from Liberia to an Atlanta hospital earlier this month. “But Ebola has been in our freezer for quite some time.”
He chuckles and then hesitates. “I’m not sure if we want to advertise that or downplay it.”
To get to the freezers filled with Ebola or the monkeys infected with the virus, you have to navigate layers of security at the Galveston National Laboratory.
At the building’s entrance, a trio of laughing graduate students holding ice boxes scan cards and disappear inside.
This might be the only place in Texas where no one will hold a door open for you. Southern manners go out the window when your building harbors a deadly virus. Piggybacking through a door is a punishable offense that will earn you a visit from the police.
Like white cells in the immune system scanning for invaders, 250 cameras line the entrance and hallways of the building. Poker-faced police officers sit behind the front desk wearing sunglasses. One police officer stares while a second offers a perfunctory “hello.”
“Where’s your ID? Why are you here? Who are you with?” he asks. He already has the answers. Four days before my visit, I am vetted and approved by the Galveston Police Department. The officer had a heads-up for my arrival.
Ebola, on the other hand, offers no warning.
___
Inside the human cell, Ebola gets naked. The virus sheds its coat and gets down to business, exposing its genes and using them to make new virus particles. Equally naked, the newly made viruses require a coat. Where else to get that coat but from the human? As they squeeze out of the cell in search of new targets, the virus particles steal bits of the human cell membrane, wrapping it around themselves. Freshly clothed, they jet off into the bloodstream.
___
At the lab, coats and bags pass through an airport-style X-ray machine. A metal detector scans visitors for weapons on the way into the main lobby. Galveston’s glorious, infectious history is proudly displayed across the lobby’s walls.
“Bubonic Plague in Galveston,” reads the headline from a reprint of the Galveston Daily News from 1920. “Yellow Fever on the Gulf Coast,” reads another.
Another part of the wall is dedicated to Louis Pasteur, grandfather of the germ theory of disease.
A copy of his legendary account of rabies, “Sur la Rage,” published in 1881 in France is displayed beneath the Galveston newspapers. Four years later, Pasteur saved the life of a 9-year-old boy bitten by a rabid dog by injecting the child with a weakened version of the rabies virus.
Geisbert applied that century-old idea to Ebola. His team developed a vaccine and injected it into monkeys infected with the virus. Just one shot saved the monkeys from an otherwise certain death. The same vaccine could be used to prevent infection, as well.
To make the vaccine, Geisbert took another virus called vesicular stomatitis virus or VSV, a virus from the same family as rabies, but one that causes flu-like symptoms in humans. He studded the exterior of the bullet-shaped virus with the three-pronged forks from Ebola’s surface.
This chimera looked like Ebola from the outside and with only a single injection, it protected the monkeys even though they were already infected.
Geisbert had figured out a way to trick the immune system. By thinking it had Ebola without actually being exposed to the fatal effects of the virus, the immune system could buy some time.
It could make the special molecules it needed to fight off the infection, molecules like antibodies that attach to viruses and bacteria, tagging them or neutralizing them and taking away their power altogether.
At least four other vaccines for Ebola are in different stages of development. None has been tested in humans because of a lack of commercial interest.
Geisbert’s vaccine is the only one that provides complete protection with just one shot.
“That’s a big deal,” he says from his office that looks out to the Gulf of Mexico. “In an outbreak you need something that works quickly. You don’t have time to wait for a booster shot. And needles are taboo in some of these cultures. You’re lucky if you can get a person in for one shot. Two or three? Good luck with that.”
___
To make an Ebola vaccine, you need luck and a strong bladder. When nature calls inside the Ebola lab, it will be 45 minutes before you see a bathroom.
First you walk slowly to the exit because the heavy spacesuit and ill-fitting rubber boots restrict movement to a clumsy dance like an astronaut navigating the moon. Then you stand for eight minutes in a small room as a chemical shower pummels you with ammonium, and then water, from every angle.
Next, you use a towel to dry the suit to prevent it from rotting. You detach your air supply — a bright yellow hose that hangs from the ceiling and attaches at the waist like an umbilical cord.
It takes strength and a few attempts to unzip the suit from head to waist. You tug and wrestle with the puller that extends up to the rigid plastic hood that engulfs the head. Then you step out of the boots, which are attached to the suit and peel off two layers of thick, latex gloves.
Fully unzipped, you still can’t use the bathroom. Long-sleeve cotton scrubs need to be removed and sterilized. Duct tape holding up men’s tube socks needs to be detached. Finally, you take a shower, and then you answer nature’s call.
It takes 30 minutes to repeat the ritual in reverse. Entering an Ebola lab takes longer than a surgeon preparing to enter an operating room to perform open heart surgery.
___
Ebola attacks the very cells designed to destroy it: macrophages. These large, white cells are a first line defense against viruses and bacteria. They bend over backward, literally changing shape, to engulf invaders before making a meal of them. No such luck with this virus. Instead, panicked white cells squirt out chemicals that make blood vessels loose and leaky. Ebola sneaks out of the leaky blood vessels and finds new cells to infect. The virus wins again.
___
In 1976, a lab worker in England accidentally pricked his thumb with a needle that had been used in a guinea pig infected with Ebola. He was treated with the blood of Ebola survivors in the hopes of transferring their antibodies to him.
Eight patients in a 1995 outbreak of Ebola in Congo received a similar treatment. The lab worker and seven of the Congolese patients survived.
Geisbert works with a small San Diego company, Mapp Biopharmaceutical, that has made an antibody treatment for Ebola called ZMapp. Mice were infected with Ebola. When they made antibodies against the virus, researchers picked out the specific ones that fought Ebola.
Geisbert didn’t work on ZMapp, but his team is collaborating with the company on future treatments.
ZMapp was given to the two Americans stricken with Ebola in Liberia. So far, both have survived — Writebol was released from the hospital Tuesday and Brantly Thursday.
But these are anecdotes, not properly controlled scientific studies. Without rigorous tests in humans, it’s impossible to decipher if it was the antibodies or the good supportive medical care given alongside them that saved lives.
Antibodies are the second option in the chemical fight against the virus. A third option to treat Ebola is being studied at Galveston National Laboratory. Small bits of genes that interfere with Ebola’s genes can interrupt the virus as it tries to make copies of itself.
These genes were given to animals who were later infected with the virus. The gene interrupters helped the animals fight Ebola and survive.
These genetic interrupters are a naturally occurring phenomenon and used by our own bodies when faced with Ebola. But the virus often finds a way to work around them and continue its cycle of replication.
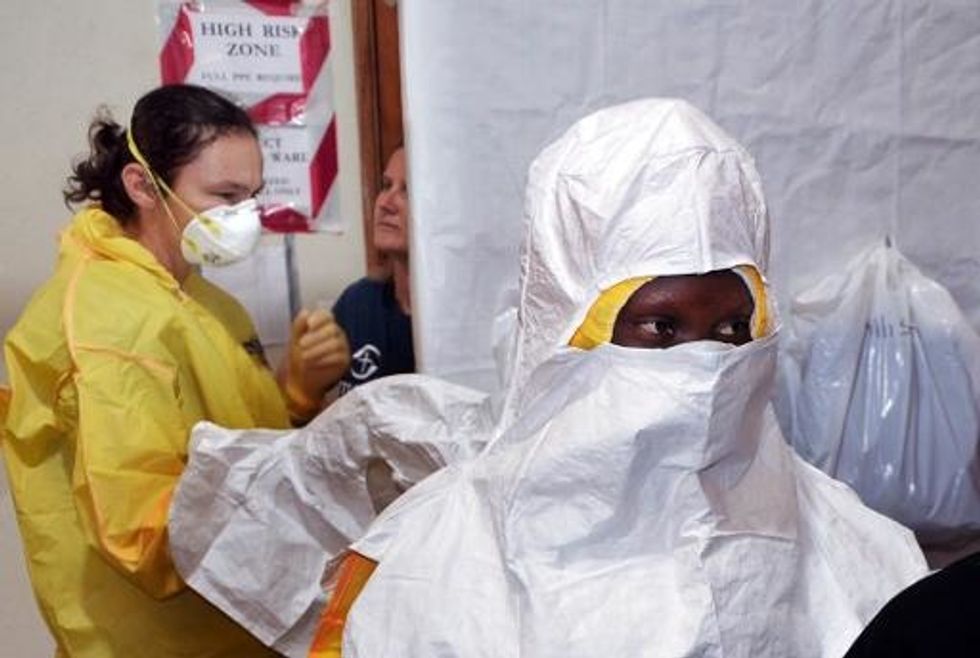
AFP Photo/Zoom Dosso
Interested in health news? Sign up for our daily email newsletter!








