Health Care Delays Squeeze Patients In State High-Risk Pools
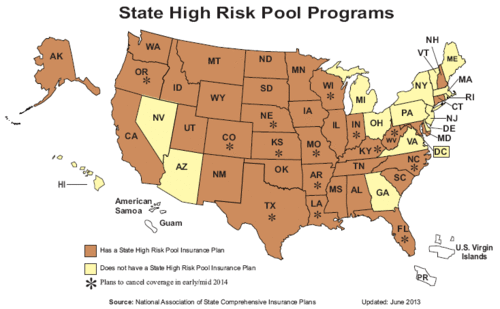
A map of states with high-risk pools for those with pre-existing conditions that deem them medically uninsurable. Similar federally funded plans under the Affordable Care Act may not be shown here. (Source: National Association of State Comprehensive Insurance Plans)
by Charles Ornstein, ProPublica.
“This is what keeps me up at night,” Tanya Case told me earlier this week.
Case is executive director of the Oklahoma Temporary High-Risk Pool, funded by the federal government to sell insurance to people denied coverage by private health insurers. Her worry is about some 300,000 people in her program and others like it who now must quickly find health insurance under the Affordable Care Act.
Many of the programs are set to close by law on Dec. 31.
By then consumers are supposed to be able to enroll in new plans that can’t discriminate against them based on their health status.
But as problems continue to bog down the federal health insurance marketplace, Healthcare.gov, it’s an open question whether people in the risk pools can get a policy in time.
“They are very frightened because many of them are undergoing chemotherapy or they’re on high-dollar drugs, and they need to make certain that they have coverage effective Jan. 1,” said Case, who is also chairwoman of the National Association of State Comprehensive Health Insurance Plans, which represents plans in 35 states.
“One lady expressed to me, ‘I’m in the middle of chemotherapy, and then I have to deal with this on top of everything else and quite frankly, I’m scared to death.’ That’s what she told me, and you hear that or a version of that quite frequently,” Case said.
People like this were supposed to among the biggest winners under the Affordable Care Act because insurers can no longer discriminate based on pre-existing conditions. As a result, the cost for many is expected to go down substantially.
Advocates say they still hope that will happen despite the current glitches.
“We’re all in this tough spot right now of guessing whether people will reasonably be able to get through” to purchase insurance on Healthcare.gov, said Stacey Pogue, senior policy analyst for the Center for Public Policy Priorities in Austin, Texas.
The concern is particularly acute in the 36 states that are relying on Healthcare.gov to process insurance enrollments. The other states and the District of Columbia are running their own marketplaces.
A spokesperson for the Centers for Medicare and Medicaid Services said the agency believes there is enough time for individuals in the high-risk pools to sign up by Dec. 15 for coverage that begins Jan. 1.
Federal officials have pledged that Healthcare.gov will be fixed by the end of November. But even if they are true to their word, Pogue said, that would only give consumers two weeks to choose a plan and enroll.
“I just don’t know yet whether it’s reasonable,” Pogue said.
Texas is one of 14 states that plan to close their high-risk pool by Jan. 1, according to Case’s group. Texas gives its insurance commissioner a bit of discretion to certify that insurance options are “reasonably available” before the state plan shuts down, Pogue said.
A federal program set up under the Affordable Care Act that serves much the same purpose (and funds Oklahoma’s program) will similarly close then. Last week, Indiana became the first state to delay its program’s closure, giving its 6,800 participants another month to find new plans. “The state of Indiana will ensure that these Hoosiers, who are facing significant health care challenges, maintain their health coverage until the problems with the federal marketplace are resolved,” Republican Gov. Mike Pence said in a statement.
Other states are considering similar moves, Case said.
Although some consumers have been successful signing up for new coverage, she said, “I would say that the majority have not been.”
In California, officials are feeling good about the transition. “There are no barriers I am aware of with people from California’s high-risk pool or anyone with pre-existing conditions getting covered for January,” said Ken Wood, a senior advisor for Covered California, the state’s insurance marketplace. “Based on the types of calls our service center has received, these individuals were reaching out the first week of October to understand their options and beginning to move through the enrollment process.”
Case said she and her colleagues in other states are encouraging consumers to shop around by calling different insurance companies — even if they cannot yet enroll on the marketplace website. They can use an online calculator to determine their eligibility for premium subsidies.
The program Case runs will shut Dec. 31 because it is funded by the federal government. But Oklahoma runs a second program that isn’t set to close right away, she said.








