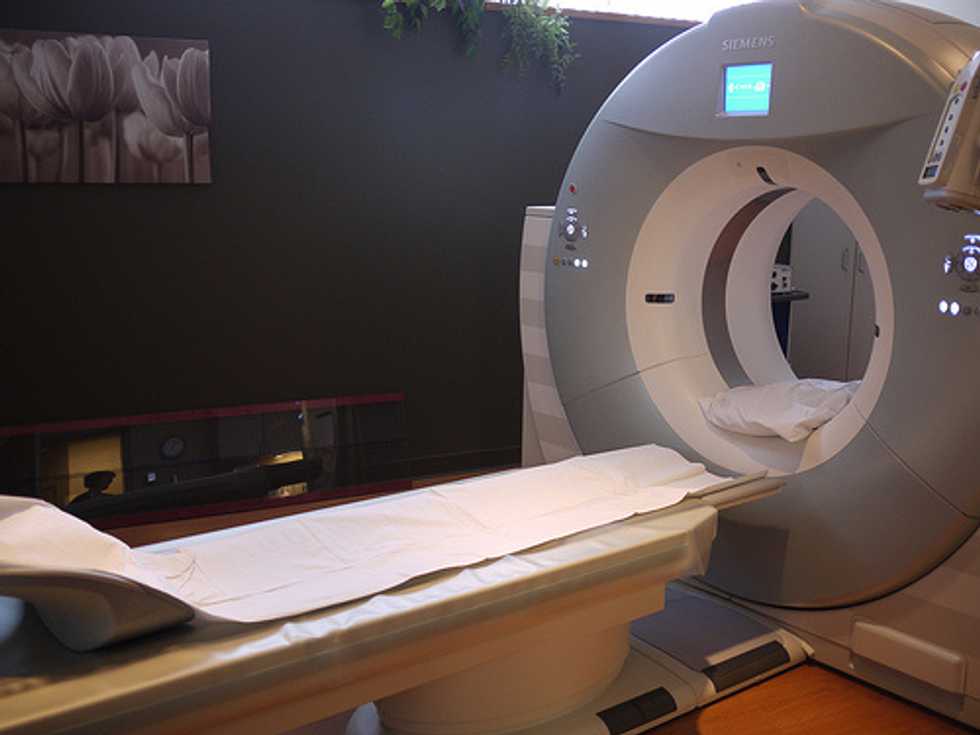
By Marie McCullough, The Philadelphia Inquirer
Two new studies add to a mountain of evidence that the U.S. Food and Drug Administration has done a poor job of making sure medical devices are safe.
The studies, in the current issue of JAMA Internal Medicine, are accompanied by commentaries that point out that the agency recognizes the need for change and is in the midst of improving the device approval system.
But critics say the FDA has an inherent conflict because of its dual role of protecting public health and encouraging medical innovation.
One of the new studies focuses on the device approval pathway known as 510(k). Created in 1976, the process allows diagnostic tests, surgical machines, heart valves, and other potentially risky devices to be cleared for marketing by submitting scientific evidence that they are equivalent to a “predicate” product already on the market. In contrast, new drugs are required to show safety and effectiveness in clinical tests.
The Institute of Medicine, an influential federal advisory panel, and advocacy groups such as Public Citizen have issued reports in recent years calling for the replacement of the 510(k) system.
For their study, researchers from the National Center for Health Research chose 50 recently marketed implantable devices — including hip replacements and bladder slings — from about 400 per year that the FDA approves under 510(k). Using an FDA database, they found that just eight of the 50 devices had filed scientific data to support their claim of being like an existing product, and only 31 of 1,105 predicate devices had done so.
“Despite the legal requirement that scientific evidence of substantial equivalence be publicly available … such information is lacking for most implanted medical devices cleared between 2008 and 2012, as well as for their predicates,” the authors concluded.
The other study, led by researchers from the Pew Charitable Trusts, focused on an FDA program that monitors the safety of high-risk medical devices such as heart stents and defibrillators. While these go through more stringent approval processes than lower-risk devices, serious problems may not show up until the devices are widely used. In recent years, for example, multiple companies have recalled defective defibrillator wiring that was placed in hundreds of thousands of patients.
The researchers found that the FDA ordered 223 post-approval studies of 158 high-risk medical devices from 2005 through 2011. However, most of the studies were too small to evaluate safety, and companies were not penalized for study delays.
When the studies revealed problems, the FDA took little or no action: It ordered only one device removed from the market, and required labeling changes for 31 products. Labeling is basically the instructions for the physician.
“One device label was changed to include the high rates of heart attacks and deaths at five years,” said Joshua Rising, a Pew researcher and study author.
While label changes may prompt physicians to add stronger warnings to the consent documents that patients have to sign, the value of labeling in ensuring safety is controversial.
“Label changes aren’t going to do anything to protect anybody,” said Noorchashm. “It’s just another layer of informed consent.”
Since December, cardiac surgeon Hooman Noorchashm of Thomas Jefferson University in Philadelphia, has waged an aggressive media and lobbying campaign to get the FDA to ban a gynecological surgery device that can spread undetected cancer.
Gynecological power morcellators device enables hysterectomies or fibroid removal to be done through tiny abdominal incisions. But in as many as one in 350 cases, the procedure spreads and worsens a rare, aggressive uterine cancer that presurgical tests can’t detect.
Anesthesiologist Amy Reed, Noorchashm’s wife and the mother of their five children, has been fighting advanced leiomyosarcoma since she underwent morcellation almost a year ago.
The FDA in April issued an unusual safety advisory to discourage physicians from using the device, and in July the agency held a hearing to decide what more to do.
But it hasn’t taken further action. (The main morcellator manufacturer has suspended sales, and the device has been disavowed by many doctors and a big health insurer.
“The FDA does not have patient safety as its primary directive,” Noorchashm said. “It wants to get innovative products to market quickly.”
Photo: Thirteen of Clubs via Flickr








